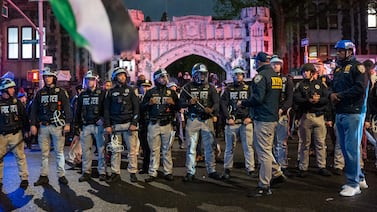There are no mask mandates and no quarantine rules in Colorado’s COVID guidance for the 2022-23 school year, but public health officials say they’re still tracking the disease and want school administrators to be open and honest with families about cases and clusters.
New guidance released Wednesday largely treats COVID like other communicable diseases, continuing a policy the state established in February at the end of the first omicron wave. At the same time, the Colorado Department of Public Health and Environment is continuing to make free rapid antigen tests widely available to schools and child care centers, both for weekly testing programs and for students to use at home.
Colorado saw high levels of COVID-19 all summer, with a sustained plateau in hospitalizations that began to decline this month. Bailey Fosdick, a member of the state’s COVID modeling team at the Colorado School of Public Health, said the lack of mitigation measures like masking may contribute to some spread in classrooms, but the combination of vaccination and recent infection should put a brake on transmission.
“Even with school starting, all of our models suggest cases and hospitalizations will continue to decline through at least the end of September,” Fosdick said. “And that’s due to the high levels of infections we saw in the spring and summer. We estimate that we still have quite a bit of immunity in the population, particularly immunity from severe disease.”
State Epidemiologist Rachel Herlihy said the new guidance aims to minimize disruptions for students and families while remaining alert for signs of clusters or higher transmission that might indicate a need for stepped-up precautions. Colorado is in a very different position than it was two years ago, she said, and that warrants a new approach.
Chalkbeat spoke with Herlihy about this approach to COVID as students return to school. Her answers are lightly edited for length and clarity.
What COVID precautions are you recommending K-12 schools take this year?
There’s no new requirements for the 2022-2023 school year. What you’re going to see in the guidance is continuing down that pathway of managing COVID-19 more like other communicable diseases. Places where previously you may have seen criteria for quarantine based on the level of vaccination in a school or the level of participation in testing, those types of things are gone now. It’s much more simplified, much more streamlined.
Quarantine is not a big focus, but you’ll see a big focus on that relationship between local public health and school districts and individual schools and really working together to identify when there are increases in transmission and when additional mitigation strategies might be needed.
An important priority in the new guidance is we do really want school administrators to continue to be transparent and share information with students and staff and parents when there are cases increasing, when there are outbreaks or there are clusters in those schools, so that those individuals have the opportunity to take extra steps to protect themselves if that’s what they want to do.
Are masks still effective against new variants?
Masks continue to be an important strategy to both protect yourself, but also potentially protect other individuals. Places where individuals might want to consider mask use would be people who are regularly in contact with people who are high risk, or people who are themselves high risk might want to wear masks. Times when mask use might also be considered would be if you’re going to be in a crowded place, especially if you have something coming up. A good example for me personally would be last year, my daughter’s graduation was coming up and transmission levels were high. Our family was routinely wearing masks for a while to minimize the chance that we would be exposed and miss her graduation and other important end-of-the-school-year type things.
So again that focus is on individual-level responsibility and decision-making.
How long should people with a positive test stay home before returning to school?
The recommendation hasn’t changed around isolation. There is that shortened isolation period of five days, and then after that the recommendation is to wear a mask. And that does continue to be an important strategy in our school guidance, that individuals who do test positive and have symptoms of COVID-19 should isolate and not be in public.
Child vaccination rates remain low in many parts of the state. What are you doing to increase those rates and what will that mean for transmission in schools?
Vaccination is obviously an important strategy to decrease the risk of transmission and also really important for preventing severe disease. We’re continuing to ensure that Coloradans have equitable access to vaccines, that schools promote vaccination alongside our local public health partners. [Almost 38% of Colorado children ages 5 to 11 are vaccinated against COVID-19, compared with 30% nationally. For children ages 12 to 17, it’s 65%.]
Some of the news about polio that you may have seen recently also reinforces the importance of other childhood vaccinations. And this is the right time for parents to be thinking about all of those vaccines as they’re getting ready to send their kids back to school.
CDPHE has stopped monitoring school-based COVID outbreaks. How will we know whether COVID is spreading in schools?
I would correct your language a little bit. Outbreaks are still reportable. We’re still very closely monitoring the data and working with our local public health partners who are working with schools to identify increases in transmission, increases in absenteeism in a way that is now more closely aligned with what we do with other communicable diseases. You may remember norovirus outbreaks that occurred before the pandemic and influenza outbreaks that occur in school. And so this approach is really about aligning our approach with COVID-19 to the approach we take with those other communicable diseases.
So what types of things would flag an outbreak? What are you watching for?
We want school staff, school administrators to be aware and looking at their absenteeism data. That is something that they are expected to do not just in the time of COVID. Even pre-pandemic, that was an expectation, looking for clusters of cases. Are there kids or staff who have similar symptoms? Are they clustered in particular classrooms or grade levels?
At that point, they would reach out to their local public health partners just like they would for flu or other infectious diseases and get guidance from public health on whether additional mitigation strategies might be needed. It could be enhanced testing in the school once increased transmission is identified. That might be when you start doing more case investigation and contact tracing once again, or quarantine, all of those things that we’ve been doing.
Were the precautions many teachers and students took over the last two years, like quarantines and masking, unnecessary? What’s changed?
I would say that there’s both virus factors and human factors that lead us to be in a very different place right now, and so our public health response has changed. We have a population that’s largely immune either through vaccination or through previous infection.
And then the virus has also changed. We continue to see these variants evolve but even as they’re becoming more transmissible, they’re causing less severe disease. And so because of that, we’re in a pretty different place. And I think that calls for an adjusting our public health response.
Earlier in the pandemic, many schools put a lot of effort into disinfecting surfaces. Now we know that’s not a major source of COVID transmission. Are there still benefits to doing that?
You’re probably speaking to someone who’s very interested in environments being disinfected and not just for COVID purposes but for other communicable diseases. We know that disinfecting surfaces can help prevent transmission of norovirus or influenza or maybe monkeypox. As we start thinking about new challenges that are facing us, disinfection continues to be an important strategy.
Speaking of monkeypox, will there be school guidance related to that?
The CDC is very actively working on that right now and has told us that we can expect school and child care-type guidance in the next one to two weeks. Children haven’t been the population that’s been most impacted — that’s what the data is showing us. But obviously, we want to be prepared as we go back to school.
Bureau Chief Erica Meltzer covers education policy and politics and oversees Chalkbeat Colorado’s education coverage. Contact Erica at emeltzer@chalkbeat.org.